Aging is a natural consequence of living, but is losing sight an inevitable consequence of aging? In this age of treatable this and replaceable that, we are unwilling to accept the loss of any function, particularly visual function. From driving the car to using the computer and other technology, working on projects of interest or keeping in touch with family, we mean to keep going forever.
 Apart from cataract surgery, where the opaque lens in the eye is replaced by an artificial lens, many of the conditions which cause loss of vision with aging are at best manageable, such as glaucoma, or at worst sight-threatening such as age-related macular degeneration (AMD).
Apart from cataract surgery, where the opaque lens in the eye is replaced by an artificial lens, many of the conditions which cause loss of vision with aging are at best manageable, such as glaucoma, or at worst sight-threatening such as age-related macular degeneration (AMD).
Age-related macular degeneration (AMD)
The incidence of AMD in the age group over 65 years is approximately 15% rising to 20-25% over 80 years old. Glaucoma affects 1 in 10 New Zealanders over 40 years old, and the high incidence of diabetes in NZ means a correspondingly high incidence of loss of some vision due to diabetic retinal disease.
Macular degeneration affects the centre of the vision causing a dark patch, blank space or distorted patch in the centre of the vision. The macula is the part of the retina we use for detailed vision like reading or recognizing faces and other small objects. It also contains the neural cells responsible for colour vision and most sensitive to light, therefore loss of function of the macula also causes reduced sensitivity to light and reduces detection of contrast i.e. how well an object stands out from its background.
If the macula is damaged for whatever reason, magnification, light, and contrast become very important aids to using remaining vision effectively. Magnifying a small word on a page means the patch in the centre of the vision does not obscure as much of the word and allows more efficient use of remaining vision. Increasing the intensity of light by using a reading lamp placed a short distance from the print improves the contrast and assists the macula to function. Badly placed light creates glare and discomfort.
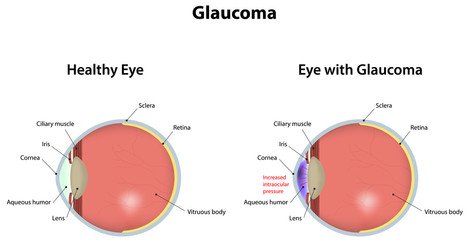
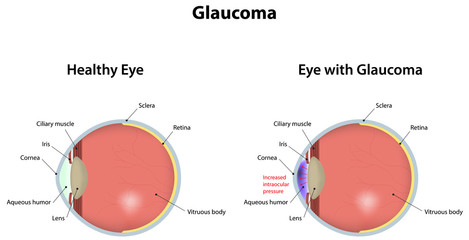 Glaucoma
Glaucoma
Glaucoma is a disease of the optic nerve which results in loss of peripheral vision. The peripheral retina also responds to poor light levels, so night vision and ability to change from light to darkness is affected.
Diabetes, high blood pressure, high cholesterol and stroke are all common contributors to loss of vision, whether central vision, peripheral or a combination of both.
These conditions do not usually come with warning flags such as pain, visible bleeding or swelling. An early sign of wet Macular Degeneration is the appearance of distortion of straight lines or a patch in the centre of the vision. Just being able to read is not an indication that all is well. There are treatments available to manage glaucoma and to limit the damage caused by some forms of Macular Degeneration.
The success of such treatments in reducing the degree of sight loss is dependent on early detection. Regular examination by an optometrist or ophthalmologist is the key to early detection.
Low vision means a partial loss of vision which cannot be restored by medical or surgical treatment or by optical means such as spectacles or contact lenses.
We often hear the term “legally blind” but we never hear “legally sighted”. The term is usually used to indicate a person’s vision is sufficiently poor to meet the criterion for membership of the Royal NZ Foundation of the Blind and therefore is bad enough to be eligible for assistance from the Foundation.
Most people who lose their vision late in life thankfully do not lose their sight to that extent. Nevertheless, any loss of vision requires changes in lifestyle which are not welcome at any age.
Naomi Meltzer
BSc., Dip Opt., P-G Dip Rehab.
Optometrist
Low Vision Consultant







phil053 - 14 years ago
After a stroke at 82 will updateing my Mums glasses help at all? She has no use of her left side, or bowels and bladder. Shes very proud and its hard to know how much she can see and how much she is guessing. Thanks, Philippa.